Login
Prostate Cancer and Treatment
Most men with prostate cancer have no symptoms.
What is Prostate Cancer and Treatment?
The prostate is a male reproductive gland that produces a fluid found in semen. Located below the bladder and in front of the rectum, the prostate surrounds the urethra - the tube that empties urine from the bladder.
Prostate cancer affects the prostate gland and may spread to surrounding structures. While most men with prostate cancer have no symptoms, physician can find prostate cancer during a regular checkup, using a combination of a blood test called a PSA and a digital rectal exam (DRE).
Nearly one in six American men will be diagnosed with prostate cancer during his lifetime. With greater awareness, prostate cancer detection is on the rise and mortality is declining. Moreover, better treatments are allowing more men to return to active and productive lives after treatment.
Treatment Options
If you have an early diagnosis of prostate cancer, there is usually a range of treatment options. These may include conservative management, radiation therapy with either external bream or brachytherapy therapy, cryosurgery and prostatectomy—surgical removal of the prostate. Your treatment options will depend on a number of factors, including the stage of the disease, your age and health or personal preference.
To minimize rectal injury during prostate cancer radiation therapy, ChristianaCare is introducing the use of the SpaceOAR (Organs at Risk) System.
Radiation therapy not only destroys prostate cancer cells but can also damage cells in the rectum and surrounding tissues.
SpaceOAR hydrogels are injected in a minimally invasive procedure to push the rectum away from the prostate and out of the high-dose radiation field, helping to minimize rectal injury and improve outcomes. The biodegradable gels are safe to use and dissolve after treatment leaving nothing behind.
If your prostate cancer has comes back and metastasized (spread to other areas of your body) and you have been treated with other therapies in the past, we are offering a new radiation treatment that may slow the growth of the tumors and prolong your life called Prostate Specific Membrane Antigen (PSMA) therapy. It is a radioactive targeted prostate cancer treatment performed in Nuclear Medicine and is a new treatment option for someone with prostate cancer. Ask your doctor if this therapy may be suitable for you and ask for a referral to Nuclear Medicine to learn more.
Prostatectomy
The gold standard treatment option for men under 70 with early-stage, organ-confined cancer is surgical removal of the prostate using nerve-sparing radical prostatectomy. Prostatectomy is also the most widely used treatment for prostate cancer today in the U.S.
The primary goal of prostatectomy is removal of the cancer. A secondary goal is to preserve urinary function and—when applicable—erectile function. Preservation of the nerves necessary for erections can be an extremely important goal for patients. These nerves run alongside the prostate and are often damaged when removing the prostate. A nerve-sparing prostatectomy attempts to preserve these nerves so that the patient may be able to return to his prior erectile function.
Types of Prostatectomy
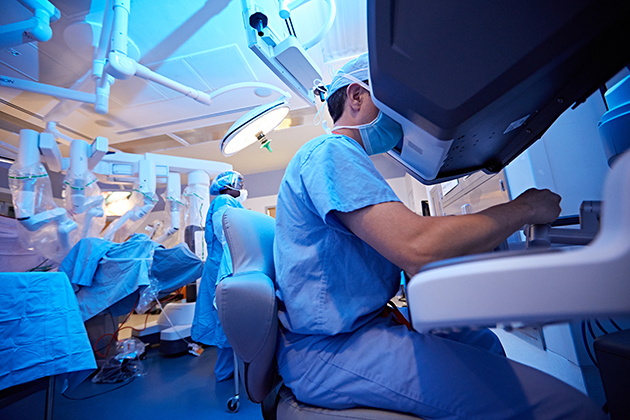
Approaches to this procedure include traditional open surgery, conventional laparoscopic surgery or da Vinci prostatectomy, which is a robot-assisted laparoscopic surgery.
With a traditional open procedure, your surgeon uses an 8-10 inch incision to access the prostate. This approach often results in substantial blood loss, a lengthy, uncomfortable recovery and a risk of impotence and incontinence.
Conventional laparoscopy uses a specialized surgical camera and rigid instruments to access and remove the prostate using a series of small incisions. This approach provides your surgeon with better visualization than an open approach. In addition, it provides the benefits of minimally invasive surgery.
Despite these advantages, conventional laparoscopy relies on rigid instruments and standard 2D video, technical limitations that can be challenging for the surgeon. Because of these drawbacks, conventional laparoscopy doesn’t lend itself well to complex procedures like prostatectomy. Therefore, very few urologists use this approach for prostatectomy. Moreover, neither laparoscopy nor open surgery can provide adequate visualization for a very precise, nerve-sparing prostatectomy.